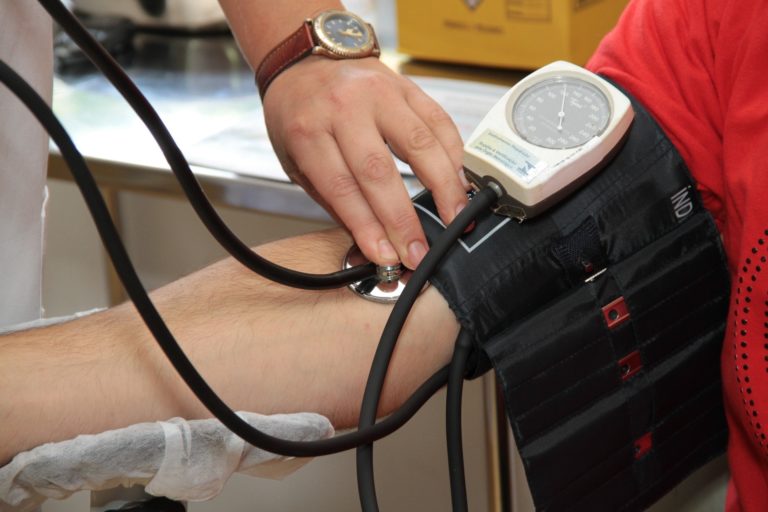
Did you know almost 3 million people in the UK have been diagnosed with chronic kidney disease (CKD)? Today is World Kidney Day and we’re highlighting how the Wearable Clinic research project at the University of Manchester, funded by EPSRC, is helping patients with CKD to monitor their own blood pressure.
It’s common for people with CKD to have high blood pressure: approximately two thirds of patients are affected. High blood pressure is often called a ‘silent disease’ because there are typically no symptoms – you can’t always ‘feel it’. But if it’s left untreated, it can lead to heart failure, stroke and further damage to the kidneys.
Therefore, it’s vital for people with CKD to manage their blood pressure and have regular, accurate measurements to detect any problems at any early stage, and prevent them from getting worse.
These measurements often aren’t as accurate as they could be. Blood pressure changes throughout the day, so having one measurement doesn’t necessarily reveal the full story about a patient’s blood pressure. Also, people often feel nervous about visiting medical settings, meaning that readings are often higher in clinic than when taken elsewhere: the so-called ‘white coat’ effect.
How can we get a clearer picture? One solution is to ask a patient to wear a monitor for 24 hours that takes measurements as they go about their everyday life.
This is where the Wearable Clinic comes in. We are designing intelligent applications for wearable technology that measure and use blood pressure readings taken outside the clinic as part of care for people with chronic kidney disease. These readings are automatically sent to the patient’s care team and integrated into their care plan.
Using state-of-the-art techniques, we detect when conditions are suitable for taking accurate readings and minimise disruption to patients.